Heart disease and autoimmune disorders can be related through various mechanisms, and the relationship between them is complex. Here are some ways in which they may be connected:
1. Inflammation:
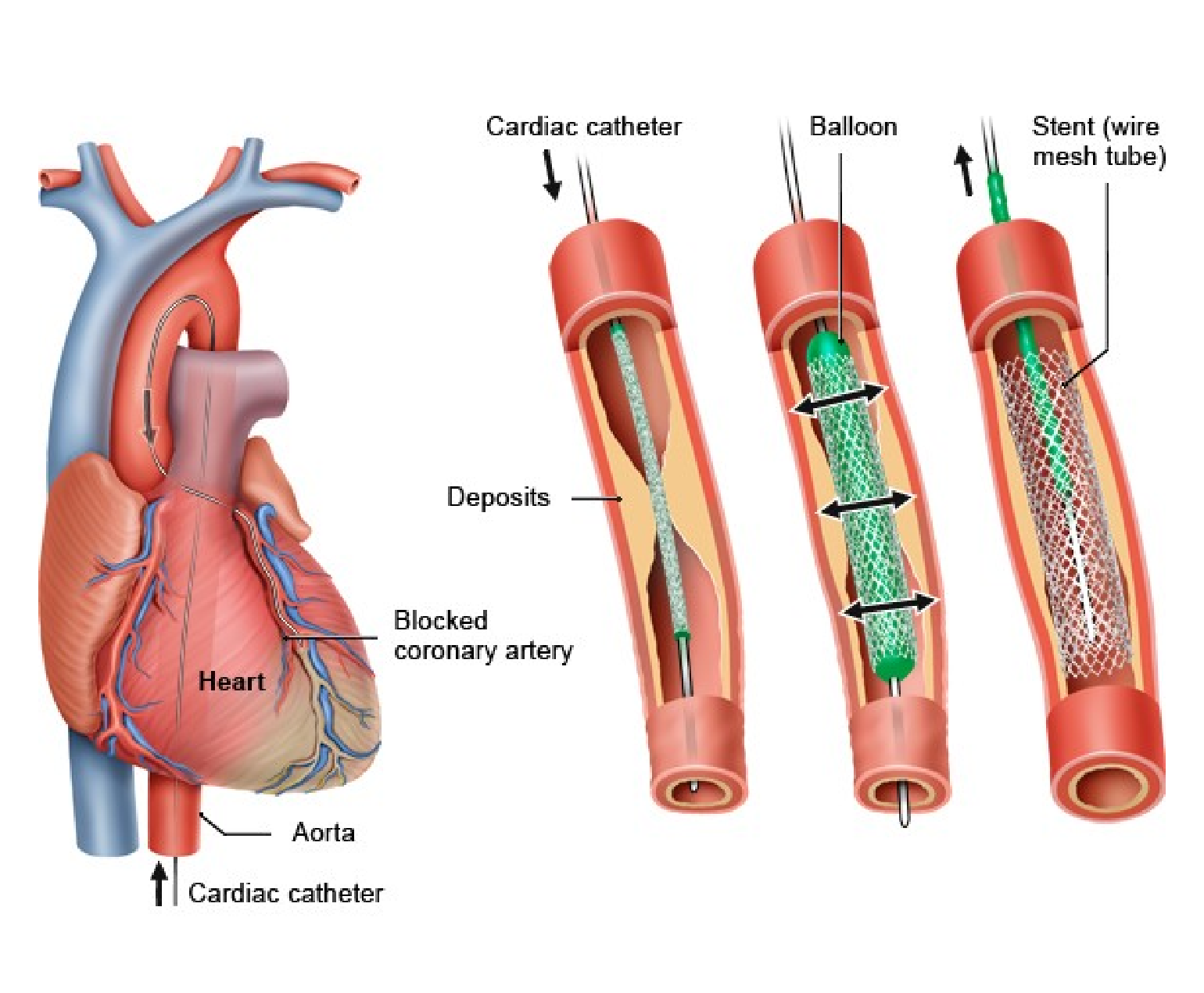
Autoimmune disorders often involve chronic inflammation as the immune system attacks the body’s own tissues. Inflammation plays a critical role in the development and progression of atherosclerosis, a condition where plaque builds up in the arteries, potentially leading to heart disease.
2. Autoimmune Myocarditis:
Some autoimmune disorders can directly affect the heart muscle. For instance, autoimmune myocarditis involves inflammation of the heart muscle, and conditions like rheumatoid arthritis and lupus have been linked to an increased risk of myocarditis.
3. Vasculitis:
Certain autoimmune disorders, such as systemic vasculitis, can affect blood vessels. Vasculitis can lead to inflammation and damage to the blood vessel walls, potentially impacting blood flow to the heart and contributing to cardiovascular complications.
4. Shared Risk Factors:
Both autoimmune disorders and heart disease may share common risk factors. For example, smoking, obesity, and a sedentary lifestyle can contribute to both autoimmune disorders and heart disease.
5. Autoimmune Diseases with Cardiovascular Involvement:
Some autoimmune diseases specifically involve the cardiovascular system. For instance, antiphospholipid syndrome is an autoimmune disorder that can cause blood clots, affect the arteries and veins, and increase the risk of heart attacks and strokes.
6. Treatment Effects:
Medications used to treat autoimmune disorders, such as corticosteroids and immunosuppressive drugs, may have cardiovascular side effects or affect traditional cardiovascular risk factors.
7. Genetic Factors:
There may be shared genetic factors that predispose individuals to both autoimmune disorders and heart disease. It’s important to note that while these connections exist, not everyone with an autoimmune disorder will develop heart disease, and vice versa. Additionally, the relationship between autoimmune disorders and heart disease can vary depending on the specific autoimmune condition.
Patients with autoimmune disorders should be monitored for cardiovascular risk factors, and healthcare providers may need to collaborate to provide comprehensive care. This often involves coordination between rheumatologists, cardiologists, and other specialists to address both the autoimmune component and potential cardiovascular implications. Regular check-ups, a healthy lifestyle, and appropriate medical management are essential for individuals with both autoimmune disorders and heart disease risk factors.